In the span of 36 hours, I found out that my anti-anxiety medication had interfered with my hormonal birth control, that there was a possibility that I could be pregnant, and that I immediately needed to get a copper intrauterine device (IUD) inserted in my uterus in order to prevent pregnancy.
To say that I was overwhelmed would be an understatement – nothing could have prepared me for the leaps and hurdles I would encounter while trying to get a copper IUD inserted in the next 36 hours with McGill international student health insurance offered with International Student Services (ISS). I write this guide hoping that no one else finds themselves in a similar situation without any knowledge of what to expect.
I was, and am, immensely privileged in that I had the funds necessary to pursue this route, as well as a good support network around me. Between the doctor consultation, the IUD itself, antibiotics, probiotics, and the gynecologist visit: it cost $435, $300 of which had to be provided in cash. (The $20 probiotics that I decided to buy were not prescribed by a doctor, and therefore not under the purview of Blue Cross.) A portion of this is reimbursable with Medavie Blue Cross international student insurance, but I had to pay the full amount up front. For many, I know this is not possible, and the fact that our health insurance is shit (more on that later) is unacceptable.
Nothing could have prepared me for the leaps and hurdles I would encounter while trying to get a copper IUD inserted in the next 36 hours with McGill international student health insurance offered with International Student Services (ISS).
How it started.
Those who have been medicated for a mental illness understand the absolute shit show that is tapering off medications. Antidepressants, which I’d been on since the fall of 2019, never fully worked for me. Yes, they reduced the chance of me having an anxiety attack, but they never addressed the all-consuming compulsions that have characterized my OCD since I was in middle school (or my skin-peeled thumbs – another common characteristic of the illness). So, when my psychiatrist in the United States prescribed me a mood stabilizer that she thought would improve my condition – without the side effects I dealt with on antidepressants – I was hopeful.
I followed her instructions, lowering my dosage of the antidepressant fluvoxamine. I began taking the mood stabilizer oxcarbazepine late Friday night. I took it again Saturday night. On Sunday morning, when I decided to search up the medication online, just for the heck of it, my heart fucking flipped – oxcarbazepine was known to interfere with hormonal birth control pills.
For many reasons, the burden of preventing pregnancy usually falls on the person with a uterus in sexual relationships where semen is also involved. Yes, people with penises can wear condoms, but they aren’t completely foolproof. And while clinical trials for hormonal contraceptives made for people with penises are ongoing, they are not yet available to the public. So, many people with uteruses take on the responsibility of using a form of hormonal birth control, all of which come with numerous side effects. The pill can cause depression, migraines, and increase your risk of blood clotting (while the pill was in its early stages of development, the dosage of estrogen within the pills was much too high, and 11 people taking it died from blood clots). The implant can cause users to experience long-term bleeding; the shot can also cause long-term bleeding, as well as depression and nausea; and the IUD, though extremely effective, is fucking painful to insert.
The best type of birth control for me had been the pill – I hadn’t experienced the worst of its side effects, and I was good at taking it on time every day. In the past, I had thought about getting a hormonal IUD but decided against it, as I was scared and uncomfortable at the thought of the insertion procedure. But once I found out that there was a possibility I could be pregnant, my comfort was the least of my worries. I was willing to sacrifice anything to ensure I wasn’t pregnant, and honestly, I’ve always been pretty open about the fact that I would definitely get an abortion if I found out I was.

Making a next-day appointment.
I spent that Sunday talking to pharmacists, first at the Jean Coutu on Parc Ave. at 8 a.m. to make sure there definitely was an interaction (there was), then calling the CVS back home to confirm at 9 a.m., and finally at the Jean Coutu on Saint Catherine Street West around 10 a.m. where I tried to buy Plan B.
The pharmacist there recommended I didn’t buy an emergency contraceptive pill, and I think they were right to do so. I had had sex twice in the past seven days, once on the Monday prior, and once that Wednesday. Although I had been absolutely protected by the pill at that time, it was unclear if it would still protect me, given the fact I’d taken interfering medication twice in the past 48 hours, and that condoms are not always effective. To be completely sure I had not conceived, they recommended that I get the copper IUD.
Some may not know that the copper IUD is the most effective method of emergency contraception out there, lowering one’s chances of getting pregnant by 99.9 per cent if inserted within five days of unprotected sex. While oral emergency contraceptives may be preferable due to their non-invasive nature, they only work well up to three or five days after unprotected sex, depending on whether you take the pill with levonorgestrel, also known as “Plan B,” “the morning after pill,” etc., or the one with ulipristal acetate, also known as “ella,” respectively. Meanwhile, a copper IUD can prevent pregnancy up to seven days after unprotected sex (though Planned Parenthood’s website says up to five days).
However, a barrier against getting the copper IUD is that it’s more expensive than oral emergency contraceptives, which cost around $20-$30 (at least in Quebec) when your insurance doesn’t cover them. And it’s important to note that emergency oral contraceptives are not covered under ISS, while IUDs are – albeit only up to $50. Once I get reimbursed from Blue Cross, I will have, in effect, paid $35 for the IUD, as it cost $85 upfront, which is still more expensive than Plan B, but only by $5-$15. The copper IUD can then be used as contraception for up to five years, which can save you money in the long run – Blue Cross only covered 80 per cent of my roughly $25 monthly pack of pills.
I was undoubtedly scared of getting an IUD. But the idea of being pregnant was scarier.
Trying to find a place that could insert it on Monday, the next day, I made calls to at least 10 different clinics. I was on hold with 811, trying to talk to an English-speaking nurse, for more than 45 minutes. I spent almost an hour and a half in total on the phone, trying to find a clinic that could schedule me in for a same-day appointment.
When I finally did get off hold and talk to a nurse at 811, they were actually pretty helpful. I was given a list of clinics nearby that offered same- or next-day copper IUD insertion, and I called one asking for an appointment on Monday morning. Tuesday was not an option – I had had sex the Monday night prior. Although the first place I called was full, I asked for a recommendation for another clinic offering same-day insertion, and I was able to schedule an appointment at Clinique Médicale Maisonneuve-Rosemont for Monday morning at 9 a.m. I could finally breathe.

Clinique Médicale Maisonneuve-Rosemont is an interesting place. Located in a building with multiple medical offices and a Familiprix, the clinic takes requests for same-day and next-day appointments both online and via phone. Since I did not have a RAMQ (Quebec health insurance card), I could not register for a walk-in appointment online, but I was able to book an appointment by calling the front desk at 514-257-7000.
This clinic – as well as many other clinics shown online through the Quebec government’s website – do not display a great deal of information regarding their services online, and calling them to confirm what they offer is often necessary. The clinics shown online via the Quebec government’s website are in French, and Google Translate is, of course, not always the best. I made do with Google and my (limited) French, but if there is someone you trust who knows French well, ask them for help. It will make the whole process so much easier.
Other clinics I was recommended in Montreal include Clinique angus (they take calls for walk-in appointments the next day beginning at 5 p.m., but if you’re an international student like me, call their regular number at 514-807-2333); Clinique en route – gare centrale (the nurse informed me that they would take calls for walk-ins beginning at 7 a.m. on Monday, 514-954-1444); and Clinique médicale des 2 tours (which you can call for a walk-in appointment the next day beginning at 6 p.m., 514-954-4444).
A barrier against getting the copper IUD is that it’s more expensive than oral emergency contraceptives, which cost around $20-$30 […] when your insurance doesn’t cover them.
The insertion procedure.
I woke up early Monday morning, nerves racing in anticipation of the procedure (It was probably also a result of not having taken any medication for my anxiety the night before). Unmedicated and scared, my boyfriend drove me 25 minutes from the McGill area to the clinic, located near the Olympic stadium. We parked, he held my hand, and we found the clinic inside the medical complex. Like the receptionist had said, it was located at the end of the hallway, on the right – bureau 60.
I brought with me everything I could possibly think of needing – Advil, a water bottle, my passport and IDs, a printed out copy of my insurance card, my debit card, and $200. Because of the type of insurance I had, the receptionist told me on the phone earlier that I’d need to pay upfront in cash, and get reimbursed by Blue Cross later. I stumbled in at the front desk, speaking a mix of English and (extremely) limited French. Sitting with my boyfriend in the clinic, we waited about 10 minutes until a nurse called us in.
This was probably the most confusing part – although the clinic says online that they offer services in both French and English, some who work there do not speak the latter. With the help of my boyfriend (who knows more French than I do), and another nurse, we were fortunately able to convey the reason I was there and the situation I was in, and they sent me to a different room in the clinic where we waited for a doctor.
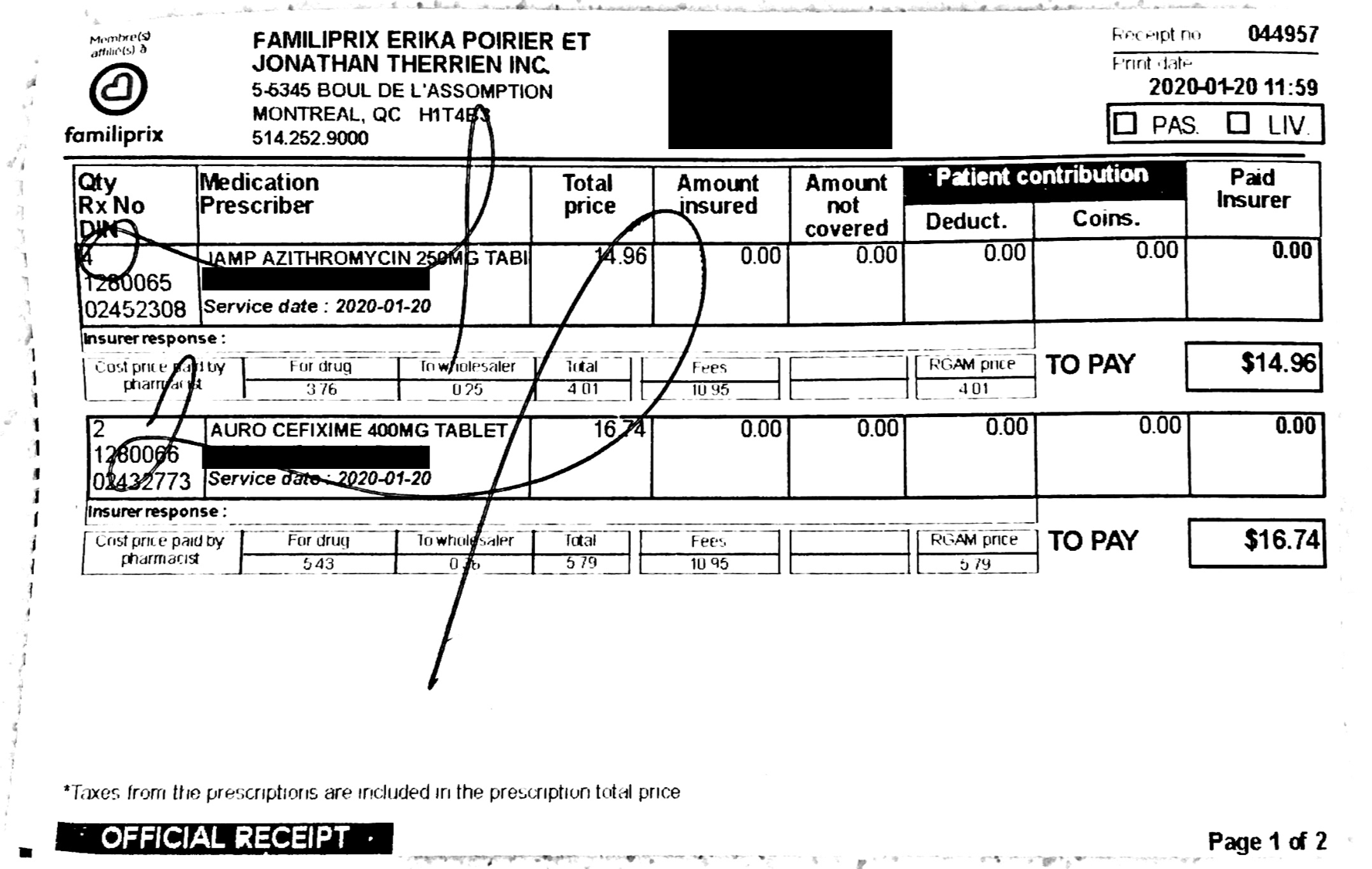
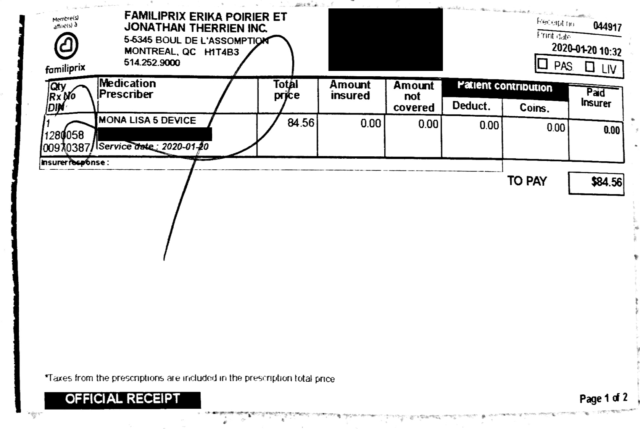
After relaying the days I had had sex and when I began oxcarbazepine, the doctor agreed that a copper IUD would work for me as emergency contraception. I was lucky, they said, because the gynecologist that performed insertions was in today. After giving me a prescription for the Mona Lisa copper IUD, a receipt for my insurance company, and a card displaying the location of the gynecologistís office – just upstairs in the same medical complex – they sent me along to Familiprix to buy the contraceptive itself (which was about $85). This hadn’t been a part of my initial calculations, and when I used my Canadian debit card to pay for it, I couldn’t purchase it – most likely due to the daily purchase limit on my account. (So if you’re ever in my position, it’d be a good idea to check your account limits – I ended up needing to use my American card.)
We took the elevator to the third floor, and I explained my situation, once again, to the receptionist. They had to confirm with the clinic downstairs, but after they did, they penciled me in for an appointment. It was a small room, filled with families waiting to see the doctor. About 30 minutes after I sat down, the gynecologist called me in.
My boyfriend and I sat in the two chairs in front of their desk. The gynecologist unwrapped the box and explained the different parts of the IUD to me, telling me that before the procedure, I would have to be swabbed and tested for gonorrhea and chlamydia – apparently if you insert an IUD and have those STIs, it’s not good. I would also have to take antibiotics to treat gonorrhea and chlamydia, regardless of what the test results were, just in case.

I felt lucky; the gynecologist said they’d never performed an insertion that resulted in infection, and that they’d done this procedure for awhile. Before I knew it, I was lying down on the table, my feet in stirrups, tightly squeezing my boyfriend’s hand. I’m not going to lie, it hurt pretty bad. Apparently if you’ve never given birth before it hurts more, and I certainly hadn’t. The worst moment was when they pinched my cervix, which is necessary in order to insert the IUD into my uterus. It felt like an instant, intense period cramp, and I was in pain. I’d told myself I’d try not to scream during the procedure, but it fucking hurt at that point.
Fortunately, it’s a pretty short procedure, all done in about two minutes (though it felt like forever in the moment). I lay on the bed for a minute or two, trying to gather my sense of self. A bit of blood had stained the bed I was laying on. I’ve always had low iron, and for the whole hour after the procedure, I felt extremely nauseous. I ended up sitting outside the office on the ground with my head between my knees while my boyfriend paid – antibiotics for gonorrhea and chlamydia ($30), and, as my boyfriend recommended, we bought some probiotics ($20). That turned out to be a really good decision; the antibiotics absolutely destroyed my digestive system. I can’t tell you how much I shit the following days.
I don’t want my story to make you think everyone will have a terrible experience getting an IUD. People’s bodies react in different ways; for some it’s easier, for some it’s more difficult. I’ve heard that some can even go back to work right afterwards.
Needless to say, that was not the case for me. While my experience wasn’t completely terrible, it was more painful than I expected. I had to stay home for the next two days, and the cramps and shits got intense. I won’t go into detail, but I’m sure you can imagine. What helped me most was the probiotics, taking two Advil every eight hours, and a hot water bottle. If you don’t have one, take an old, clean sock and fill it with rice. Then heat it up in the microwave for 30 seconds; it will feel – and work – the same as the hot water bottle you buy at the pharmacy.
I made calls to at least 10 different clinics. I was on hold with 811, trying to talk to an English-speaking nurse, for more than 45 minutes. I spent almost an hour and a half in total on the phone.
The aftermath.
I stopped spotting and experiencing cramps roughly a week after the procedure. I’m supposed to take a pregnancy test approximately two to three weeks after the IUD insertion to make sure I didnít conceive. (If you don’t want to wait until your next scheduled period to take a pregnancy test, you can take one 7-14 days after having sex – but it may not be as accurate as if you wait until the week your period is supposed to start.) And in two months, I have an appointment back at the gynecologist for them to check up on my IUD. The cramps have subsided for the moment, but we’ll see how my first period with a copper IUD goes; many people using this form of birth control report heavy cramps and bleeding, as well as irregular periods.
When I tried to have my expenses reimbursed, the Medavie Blue Cross office on McGill College Avenue informed me that they do reimbursements online and via their mobile app now – not in person. I used to be able to walk to their location next to Dormez-Vous on Sherbrooke and get my birth control prescriptions reimbursed there, but that location closed in November 2019. As it takes five to seven business days for the claim to be processed, I found out five days after I submitted my claim exactly how much I would be reimbursed.
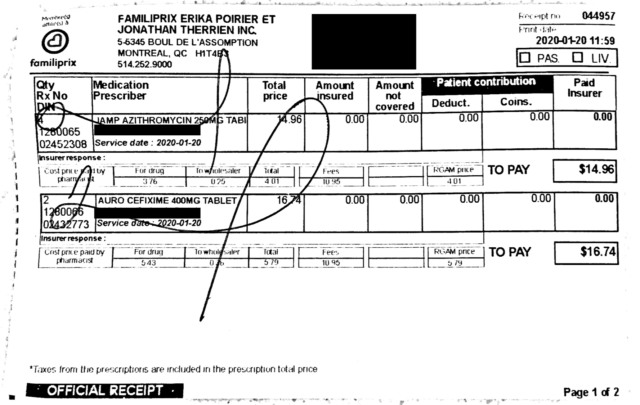
The approximately $415 in prescriptions and doctors visits that I submitted to Blue Cross, as I suspected, was not entirely reimbursable. While the visit to the gynecologist ($100) was completely covered, the initial doctor consultation was not – I paid $200 in cash for it, and Blue Cross says they will cover $106.20 of it. As I mentioned earlier, for the copper IUD itself, they only cover $50 in IUD purchases (meaning I will have paid $35 for it). While $35 for a copper IUD is not as expensive as the hormonal alternatives – one hormonal intrauterine system (IUS) in Quebec costs around $325, meaning that an international student who purchases one may still have to pay around $275 for it after getting reimburse – it is still a barrier, and even more so if one wishes to purchase the hormonal IUS. (And especially considering the fact that these costs had to be paid upfront.)
Because of the type of insurance I had, the receptionist told me on the phone earlier that I’d need to pay [$200] upfront in cash, and get reimbursed by Blue Cross later.
As for the gonorrhea and chlamydia antibiotics, they were each reimbursed by 80 per cent. Together, they cost approximately $30, and Blue Cross says they will pay $25 for it. All in all, Blue Cross will pay $280 out of the $415 total expenses (excluding the probiotics).
According to VP Finance Samuel Haward, both he and the SSMU Mental Health Commissioner have met with the directors of ISS and Student Services to discuss the review of international student health insurance and negotiate a new plan with Blue Cross. Haward stated that student associations have little control over the plan, and that it is under the purview of Senate and Procurement Services. Fortunately, this review may be happening sooner rather than later – it is set to occur in 2020-2021.
As international student insurance is set to be reviewed, I implore both Senate and Procurement Services to consider the extensive barriers that international students face under this current plan. Upfront costs, especially unexpected ones paid in times of emergency, disproportionately affect lower-income students. If someone who is in my position is not able to pay these costs, there is the possibility that they could become pregnant, and that is unacceptable.
I implore both Senate and Procurement Services to consider the extensive barriers that international students face under this current plan. Upfront costs, especially unexpected ones paid in times of emergency, disproportionately affect lower-income students.